WHS Oral Abstracts
(WHS-K4.02) INTRAVESICULAR CYTOKINE PROFILING OF STAGE IV PRESSURE ULCERS TREATED WITH NPWT VS. NPWT AND PORCINE EXTRACELLULAR MATRIX DRESSING
Thursday, May 16, 2024
9:15 AM - 10:15 AM East Coast USA Time
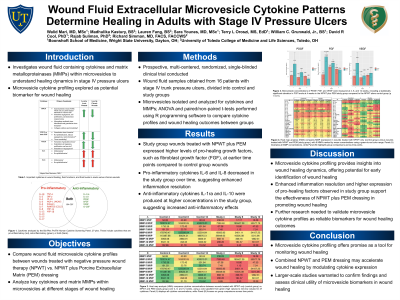
Background: Extracellular vesicles (EVs) are involved in all phases of wound healing. They carry cytokines, which possess a wide range of pro-inflammatory and pro-healing functions. While inflammation is critical in wound healing, it must be resolved so that wounds can progress to proliferation and remodeling. Otherwise, wounds become chronic. The purpose of this study is to analyze intravesicular cytokines in wound fluid to understand how healing and non-healing wounds behave at the molecular level when treated with negative pressure wound therapy (NPWT) versus a combination of NPWT and Porcine Extracellular Matrix dressing (Oasis Ultra).
Methods: Wound fluid samples were obtained from 16 patients with stage IV trunk pressure ulcers. The patients were divided into two groups (n= 8 in each): a control group on NPWT alone and a study group on NPWT plus Oasis Ultra. A canister of patient wound fluid was collected from the NPWT device (wound VAC) every four weeks over the course of the 12-week study. Microvesicles were isolated and analyzed for concentration and content. The following were assayed: growth factors, proinflammatory interleukins and molecules, anti-inflammatory interleukins, and enzymes.
Results: In previous experiments, we found that the overall wound healing rate was significantly higher in the Porcine Extracellular Matrix study group compared to the control group (p < 0.05), as determined by wound size at 12 weeks. Study group wounds also healed faster. In our molecular data analysis, wounds in the study group expressed higher intravesicular pro-healing growth factor concentrations earlier in the study compared to wounds treated with NPWT (control) alone. For example, the intravesicular fibroblast growth factor (FGF) concentration at 4 weeks in the study group was statistically significantly higher than the control group (112.93 pg/mL vs. 28.51 pg/mL, p< 0.01). As wounds progressed toward healing, the EV concentration of proinflammatory molecules such as IL-5, IL-6, IL-8, IL-12, IFN-γ, and TNF-α decreased in the study group over time and were lower than control group levels by 12 weeks. Anti-inflammatory molecules IL-1ra and IL-10 were produced at higher concentrations in the faster healing study group as compared to the NPWT only group.
Conclusion: Wound healing is a regulated process involving both proinflammatory and inflammation-resolving mediators. Given the correlations between our molecular data and prior clinical wound healing data, our results suggest critical interactions between intravesicular cytokines and cells in the actual wound site. To our knowledge, this is the first study to successfully isolate microvesicles containing wound healing specific cytokines at multiple time intervals for a prolonged period. Intravesicular molecular profiling can help characterize wound progression, serving as a wound healing biomarker.
Methods: Wound fluid samples were obtained from 16 patients with stage IV trunk pressure ulcers. The patients were divided into two groups (n= 8 in each): a control group on NPWT alone and a study group on NPWT plus Oasis Ultra. A canister of patient wound fluid was collected from the NPWT device (wound VAC) every four weeks over the course of the 12-week study. Microvesicles were isolated and analyzed for concentration and content. The following were assayed: growth factors, proinflammatory interleukins and molecules, anti-inflammatory interleukins, and enzymes.
Results: In previous experiments, we found that the overall wound healing rate was significantly higher in the Porcine Extracellular Matrix study group compared to the control group (p < 0.05), as determined by wound size at 12 weeks. Study group wounds also healed faster. In our molecular data analysis, wounds in the study group expressed higher intravesicular pro-healing growth factor concentrations earlier in the study compared to wounds treated with NPWT (control) alone. For example, the intravesicular fibroblast growth factor (FGF) concentration at 4 weeks in the study group was statistically significantly higher than the control group (112.93 pg/mL vs. 28.51 pg/mL, p< 0.01). As wounds progressed toward healing, the EV concentration of proinflammatory molecules such as IL-5, IL-6, IL-8, IL-12, IFN-γ, and TNF-α decreased in the study group over time and were lower than control group levels by 12 weeks. Anti-inflammatory molecules IL-1ra and IL-10 were produced at higher concentrations in the faster healing study group as compared to the NPWT only group.
Conclusion: Wound healing is a regulated process involving both proinflammatory and inflammation-resolving mediators. Given the correlations between our molecular data and prior clinical wound healing data, our results suggest critical interactions between intravesicular cytokines and cells in the actual wound site. To our knowledge, this is the first study to successfully isolate microvesicles containing wound healing specific cytokines at multiple time intervals for a prolonged period. Intravesicular molecular profiling can help characterize wound progression, serving as a wound healing biomarker.

.jpeg)
