WHS Posters
(WHS-P17) EXPERIENCE USING A SYNTHETIC SKIN SUBSTITUTE FOLLOWING ACUTE BURN INJURY AT A TERTIARY BURN CENTER
Friday, May 17, 2024
7:30 AM - 5:00 PM East Coast USA Time
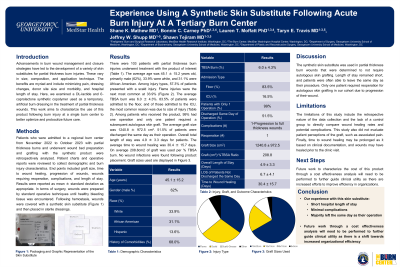
Background Advancements in burn wound management and closure strategies have led to the development of a variety of skin substitutes for partial thickness burn injuries. These vary in size, composition, and application technique. The benefits are myriad and include minimizing pain, dressing changes, donor site size and morbidity, and hospital length of stay. Here, we examined a DL-lactide and ε-caprolactone synthetic copolymer used as a temporary, artificial burn dressing in the treatment of partial and full thickness wounds. This work aims to characterize the use of this product following burn injury at a single burn center to better optimize and protocolize future care. Methods Patients who were admitted to a regional burn center from November 2022 to October 2023 with partial thickness burns and underwent wound bed preparation and grafting with the synthetic product were retrospectively analyzed. Patient charts and operative reports were reviewed to collect demographic and burn injury characteristics. End points included graft size, time to wound healing, progression of wounds, wounds requiring reoperation, complications, and length of stay. Results were reported as mean ± standard deviation as appropriate. Results There were 103 patients who underwent treatment with the product of interest. The average age was 45.1 ± 15.2 years old, primarily male (62%), 33.9% were white, and 31.1% were African American. Among injury types, 57.3% of patients presented with a scald injury. Flame injuries were the next most common at 33.9%. The average TBSA burn was 6.0 ± 4.3%. 83.5% of patients were admitted to the floor, and of those admitted to the ICU, the most common reason was due to size of injury. Among patients who received the product, 99% had one operation, and only one patient required a subsequent autologous skin graft. The average graft size was 1240.8 ± 972.5 cm2. Regarding disposition, 51.5% of patients were discharged the same day as their operation. Overall total length of stay was 4.9 ± 3.3 days for patients. The average time to wound healing was 30.4 ± 15.7 days. On average 208.8cm2 of graft was used per % TBSA burn. No wound infections were found following product placement. Discussion The synthetic skin substitute was used in partial thickness burn wounds that were determined to not require autologous skin grafting. Length of stay remained short, and patients were often able to leave the same day as their procedure. Only one patient required reoperation for autologous skin grafting in our cohort. Future work to characterize the cost of this product will need to be performed to further guide clinical utility and cost effectiveness.

.jpeg)
