Practice Innovations
(PI-027) Complex Fistula Care: An Innovative Approach to the Treatment of a Large Abdominal Surgical Wound with Multiple Enterocutaneous Fistulas Managed in the Outpatient Setting using Transforming Powder Dressing (TPD)
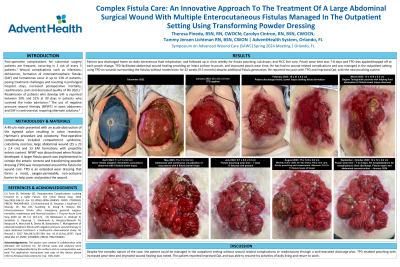
Post-operative complications for patients undergoing colorectal surgery are frequent, occurring in 1 out of every 3 patients.1 Wound complications such as infection, dehiscence, enteroatmospheric fistula (EAF) formation and hematomas occur in up to 13% of patients, posing challenges to treatment and resulting in prolonged length of hospital stay, postoperative mortality, readmissions, decreased quality of life (QoL) and pain.1
Readmission of patients who develop EAF is reported between 20 and 51% at 90 days amongst patients who survived the index admission.2 and has an associated mortality rate between 20-44%.2. The use of negative pressure wound therapy (NPWT) in open abdomens and EAF is controversial.3 Due to the complex nature and extended healing times associated with open abdominal wounds, alternative wound treatment options must be investigated.
Methods: A 40-year-old male presented with an acute obstruction of the sigmoid colon resulting in colon resection, Hartman’s procedure and colostomy. Post-operative complications included compartment syndrome, colostomy necrosis, large abdominal wound (25 x 23 x 2.4 cm) and 13 EAF formations with projectile enteric content. NPWT was discontinued when fistulas developed. A large fistula pouch was then implemented to contain the enteric content and transforming powder dressing (TPD) was incorporated for wound healing. TPD is a commercially available extended wear dressing that forms a moist, oxygen-permeable barrier that covers and protects the wound.
Results:
He was discharged home on daily intravenous fluid rehydration, and followed up in clinic weekly for fistula pouching, lab draws, PICC line care. Pouch wear time was 7-8 days, and TPD was applied weekly. He has had no complications or readmissions since discharge 42 weeks (about 9 and a half months) ago. Furthermore, he reported less pain and improved QoL when TPD and the pouching system was incorporated.
Discussion: This highly complex patient has been maintained in the outpatient setting with no complications and no readmission rates through a well-executed discharge plan. By introducing TPD treatment to this challenging abdominal wound, observable improvements in wound healing were noted with no adverse events. The patient reported improved QoL and was able to resume his activities of daily living including return to work.

.jpeg)