Laboratory Research
(LR-035) Hypothermic Storage Maintains Key Characteristics of Fresh Placental Membranes and Provides a Scaffold to Support Tissue Growth
Human placental tissues, consisting of amnion and chorion membranes, have been shown to support wound healing clinically, while pre-clinical studies have established placental membranes as a source of growth factors, cytokines, and extracellular matrix (ECM) proteins. A proprietary hypothermic storage processing technique has been developed to preserve and maintain the native characteristics of amnion (HSAM†) and chorion (HSCMº) membranes. In this study, we hypothesized that HSAM and HSCM would retain key properties characteristic of fresh amnion and chorion membranes. To evaluate this, biophysical properties of fresh and hypothermically stored placental membranes were characterized, along with their response to degradation. Additionally, HSAM and HSCM were evaluated for their scaffold functionality in vitro.
Methods:
Hypothermically stored placental membranes were compared to corresponding fresh amnion and chorion membranes (fAM and fCM) using scanning electron microscopy (SEM) and immunohistochemical staining for ECM components and key growth factors/cytokines. Functionality as a protective barrier in vitro was assessed by measuring degradation in simulated wound fluid through quantification of retained mass. Functionality as a scaffold in vitro was assessed by evaluating the capacity of HSAM and HSCM to support cell attachment and growth by culturing with primary human dermal fibroblasts.
Results:
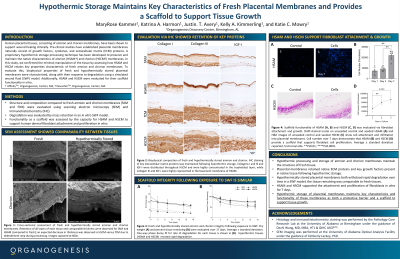
Following processing and hypothermic storage, placental membranes retained native tissue structure and ECM proteins, including Collagens I and III, which were distributed throughout HSCM and were highly concentrated in the trophoblast layer, while Collagen III was highly represented in the basement membrane of HSAM. HSAM and HSCM conserved key growth factors/cytokines present in fresh amnion and chorion, respectively. In vitro degradation studies found that both HSCM and HSAM withstood rapid degradation over time, and the tissue remaining was overall comparable with fresh tissues. HSAM and HSCM supported the attachment and proliferation of fibroblasts in vitro, with significant growth out to 7 days (p< 0.05).
Discussion:
These results highlight the hypothermic process as an effective method for processing and preserving placental membranes, and the ability to maintain key characteristics of fresh tissues and the functionality of these membranes as both a protective barrier and a scaffold to support tissue growth.

.jpeg)