WHS Posters
(WHS-P80) Adjunctive Biofilm management thru the mitigation of microvascular hyperpermeability; A Theory
Friday, May 17, 2024
7:30 AM - 5:00 PM East Coast USA Time
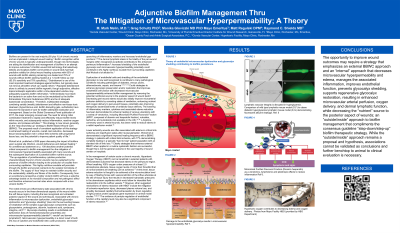
Biofilms are implicated in delayed healing. The 2017 Global Consensus Panel publication established "step down, step up therapy" and “the need for strong initial combination treatment to rapidly and effectively reduce biofilm levels within wounds." Wolcott et al. published a 2008 paper discussing a potential critical component to biofilm management thru the mitigation of microvascular hyperpermeability associated with wounds and the deprivation of biofilm nutrients. The pro-inflammatory state occurs in 3D within soft tissues, including the posterior aspect of the wound, with associated microvascular and endothelial dysfunction and “glycocalyx shedding” (loss into the surrounding tissues of complex sugar components such as glycoproteins, proteoglycans, albumin, hyaluronic acid, etc). Shedding results in endothelial cell dysfunction (loss of mechanotransduction), diffuse microvascular hyperpermeability, resulting in loss of nitric oxide production, decreased inflammatory marker quenching, increased endothelial gap junctions. Dermal lymphatic stasis in peri-wound margins contributes to enhanced periwound inflammation. Endothelial glycocalyx and microvascular hyperpermeability potentially contribute to highly nutritious exudate from surrounding capillaries, enhancing biofilm sustainability. Dysfunction of endothelial cells and shedding of the endothelial glycocalyx is well recognized to contribute to pathological conditions including diabetes, venous ulcers, atherosclerosis, sepsis, trauma. Could strategies to enhance glycocalyx preservation and/or restoration that improve endothelial cell function with decreased microvascular hyperpermeability enhance biofilm management by removing potential nutritional source to wound beds? The lowering of inflammatory markers, cytokines and associated edema reduction has been demonstrated to enhance healing of venous ulcerations with a variety of venotonics, including micronized purified flavonoid fraction, rutosides and sulodexide. L-Arginine has been noted to reduce edema in a rabbit reperfusion model. The opportunity to improve outcomes may require a strategy that emphasizes an external biofilm and an “internal” approach that decreases microvascular hyperpermeability and edema, manages the associated inflammation, improves endothelial function, improves microvascular arterial perfusion, oxygen delivery, and dermal lymphatic function, while decreasing the “nutrient” source to the posterior aspect of wounds; an “outside/inside” approach to biofilm management that compliments the consensus guideline “step-down/step-up” biofilm therapeutic strategy. This remains a hypothesis, further benchtop to animal to clinical evaluation is necessary.

.jpeg)
