WHS Posters
(WHS-P68) Representation Of Patients With Renal Disease In Wound Healing Intervention Studies
Friday, May 17, 2024
7:30 AM - 5:00 PM East Coast USA Time
Background: Patients with renal failure and chronic kidney disease (PWRD) have profoundly impaired wound healing due to various factors including comorbid arterial disease, poor nutrition, uremia, anemia, and neuropathy. Diabetic foot ulcers (DFUs) are a common chronic wound seen in this population. PWRD also have higher risk of calciphylaxis, a rare but highly morbid wound caused by uremic arterial calcification. Despite these factors, PWRD are commonly excluded from wound healing studies. The purpose of this review is to quantify the representation of PWRD in studies on DFU and lower extremity calciphylaxis interventions. We also aim to evaluate differences in the efficacy of interventions between patients with and without renal impairment.
Methods: A systematic review was conducted using PRISMA guidelines to investigate wound healing interventions for treatment of DFUs or calciphylaxis. PubMed, Cochrane, Embase, MedLine, and WebofScience databases were queried for relevant articles published from February 2013-2023. Duplicates were eliminated, and abstract and full text review were conducted. The primary outcome was inclusion of PWRD. Secondary outcomes included number of PWRD and specific wound healing parameters.
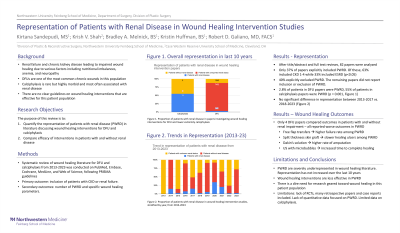
Results: The initial database search yielded 688 articles. After abstract and full text review, 82 papers were analyzed. Of these papers, only 30 (37%) included PWRD and reported the number of patients with this comorbidity. 34 papers (40%) explicitly excluded PWRD. While the remaining 18 papers did not exclude PWRD, they did not explicitly report patient comorbidities. Thus, inclusion of PWRD could not be determined. Among DFU papers, 2.8% of patients represented were PWRD. However, previously reported prevalence of renal disease among DFU patients ranges from 15-50%. For calciphylaxis papers, 55% of included patients were PWRD. There was no significant difference in representation of PWRD in 2013-2017 versus 2018-2023 (p=0.75). Only 4 papers, including one case report, compared outcomes between PWRD and patients without. Two papers on surgical interventions showed poorer results in PWRD. Chou et al. studied free flap transfers for DFU treatment and noted that 90% of failed flaps belonged to PWRD. Walters et al. investigated split-thickness skin grafts for DFUs and found that patients with slow-healing plantar ulcers were more likely to have renal disease (p=0.002).
Conclusion: PWRD experience delayed wound healing due to several factors. However, they are not well-represented in literature on wound healing interventions, with little improvement over the last 10 years. The few papers that do compare outcomes between patients with and without renal disease continue to suggest existing interventions are not effective in PWRD. There remains a dire need for investigation into wound healing treatments for these patients.
Methods: A systematic review was conducted using PRISMA guidelines to investigate wound healing interventions for treatment of DFUs or calciphylaxis. PubMed, Cochrane, Embase, MedLine, and WebofScience databases were queried for relevant articles published from February 2013-2023. Duplicates were eliminated, and abstract and full text review were conducted. The primary outcome was inclusion of PWRD. Secondary outcomes included number of PWRD and specific wound healing parameters.
Results: The initial database search yielded 688 articles. After abstract and full text review, 82 papers were analyzed. Of these papers, only 30 (37%) included PWRD and reported the number of patients with this comorbidity. 34 papers (40%) explicitly excluded PWRD. While the remaining 18 papers did not exclude PWRD, they did not explicitly report patient comorbidities. Thus, inclusion of PWRD could not be determined. Among DFU papers, 2.8% of patients represented were PWRD. However, previously reported prevalence of renal disease among DFU patients ranges from 15-50%. For calciphylaxis papers, 55% of included patients were PWRD. There was no significant difference in representation of PWRD in 2013-2017 versus 2018-2023 (p=0.75). Only 4 papers, including one case report, compared outcomes between PWRD and patients without. Two papers on surgical interventions showed poorer results in PWRD. Chou et al. studied free flap transfers for DFU treatment and noted that 90% of failed flaps belonged to PWRD. Walters et al. investigated split-thickness skin grafts for DFUs and found that patients with slow-healing plantar ulcers were more likely to have renal disease (p=0.002).
Conclusion: PWRD experience delayed wound healing due to several factors. However, they are not well-represented in literature on wound healing interventions, with little improvement over the last 10 years. The few papers that do compare outcomes between patients with and without renal disease continue to suggest existing interventions are not effective in PWRD. There remains a dire need for investigation into wound healing treatments for these patients.

.jpeg)
