WHS Posters
(WHS-P55) Review of 100 Consecutive Same-Day Discharge Hip and Knee Replacement Patients Using the PICO Dressing
Friday, May 17, 2024
7:30 AM - 5:00 PM East Coast USA Time
Introduction: Total joint arthroplasty, including total hip arthroplasty and knee arthroplasty is of the most successful and reliable procedures in orthopedic surgery to restore function and alleviate pain. As orthopedic surgery in general has evolved to more patient centric and often done in the outpatient setting, so too have total hip and total knee replacements. Delayed wound healing and wound infection continue to be one of the most common complications often with devastating effects, including repeat surgery and removal of the prosthesis. To improve the wound environment and promote healing, negative pressure dressings have been developed in recent years. The PICO system is unique in that it uses a highly absorbent sponge instead of a separate canister, and it is a disposable item. This paper outlines a retrospective review of 100 consecutive same-day discharge total hip and total knee patients specifically to review delayed wound healing, wound infections and repeat surgery with all patients using the negative pressure PICO dressing postoperatively.
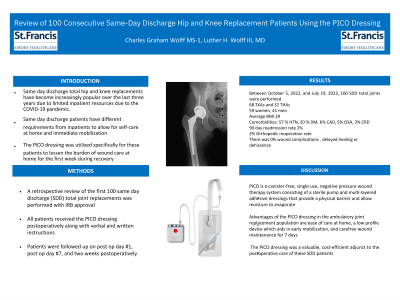
Methods: Between October 5, 2021, and July 19, 2022, 100 same-day discharge total joints were performed consisting of 68 total knee replacements (TKA) and 32 total hip replacements (THA). There were 41 men and 59 women, with an average age of 62 (range 41-77) at the time of surgery. Eighty one percent of the patients had at least one medical comorbidity including hypertension (57%), diabetes mellitus (20%), coronary artery disease (6%), sleep apnea (5%) and renal disease (3%). All patients received the PICO dressing postoperatively. The hip replacement patients had it applied immediately after wound closure on the day of surgery. The knee replacement patients had their PICO applied on POD #1 during the first physical therapy appointment.
Results: There was a 2% readmission rate during the 90-day postoperative period. One patient was admitted on POD #5 for gastritis and dehydration. The other patient was readmitted on POD #11 for weakness and anemia, work-up revealed bleeding from a GIST tumor which was resected without complication. There were no cases of DVT, PE, pneumonia or UTI. The mortality rate was 0%. With this protocol, there were zero wound related issues. Specifically, no patient developed delayed wound healing, dehiscence or post-operative wound infection. There were no repeat surgeries in this cohort for wound related issues.
Conclusion: Wound related issues continue to be one of the most common complications leading to more frequent visits, repeat procedures and patient dissatisfaction. The PICO dressing is ideal for the outpatient total joint setting where patient self-care is more common until the first follow up. In this series of 100 same day discharge patients, the PICO dressing proved to be beneficial with no wound related issues or repeat procedures and high level of patient satisfaction.
Methods: Between October 5, 2021, and July 19, 2022, 100 same-day discharge total joints were performed consisting of 68 total knee replacements (TKA) and 32 total hip replacements (THA). There were 41 men and 59 women, with an average age of 62 (range 41-77) at the time of surgery. Eighty one percent of the patients had at least one medical comorbidity including hypertension (57%), diabetes mellitus (20%), coronary artery disease (6%), sleep apnea (5%) and renal disease (3%). All patients received the PICO dressing postoperatively. The hip replacement patients had it applied immediately after wound closure on the day of surgery. The knee replacement patients had their PICO applied on POD #1 during the first physical therapy appointment.
Results: There was a 2% readmission rate during the 90-day postoperative period. One patient was admitted on POD #5 for gastritis and dehydration. The other patient was readmitted on POD #11 for weakness and anemia, work-up revealed bleeding from a GIST tumor which was resected without complication. There were no cases of DVT, PE, pneumonia or UTI. The mortality rate was 0%. With this protocol, there were zero wound related issues. Specifically, no patient developed delayed wound healing, dehiscence or post-operative wound infection. There were no repeat surgeries in this cohort for wound related issues.
Conclusion: Wound related issues continue to be one of the most common complications leading to more frequent visits, repeat procedures and patient dissatisfaction. The PICO dressing is ideal for the outpatient total joint setting where patient self-care is more common until the first follow up. In this series of 100 same day discharge patients, the PICO dressing proved to be beneficial with no wound related issues or repeat procedures and high level of patient satisfaction.

.jpeg)
