WHS Posters
(WHS-P43) FACTORS AFFECTING COMPLICATION RATES FOR CHEST WALL TUMOR EXCISION WITH PLASTIC RECONSTRUCTION
Friday, May 17, 2024
7:30 AM - 5:00 PM East Coast USA Time
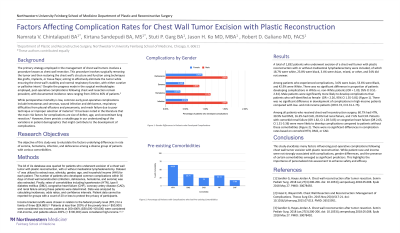
Background The main approach for treatment of chest wall tumors is chest wall resection, which can generally be carried out with minimal risk of complications including dehiscence, seroma, hematoma, and infection. However, there remains a knowledge gap in ascertaining demographic differences between patients who develop complications. Methods The All of Us database was queried for patients with excision of a chest wall tumor with plastic reconstruction, with or without mediastinal lymphadenectomy. Dataset v7 was utilized to extract race, gender, income, and comorbidity data along with respective rate of development of dehiscence, seroma, hematoma, or infection within 30 days. Results A total of 1,832 patients who underwent excision of a chest wall tumor with plastic reconstruction with or without mediastinal lymphadenectomy were included, of which 18.7% were white, 23.8% were black, 1.0% were Asian, 2.4% were mixed or other, and 54% did not answer. There was no significant difference in proportion of patients developing complications on the basis of race. While patients who self-identified as male made up a smaller proportion of total patients, they were more likely to develop complications (5.1%) than patients who self-identified as female (2.3%) (OR = 2.26, 95% CI 1.35-3.81) There was no significant difference in development of complications between patients with an annual household income of greater than $100,000 compared to patients with an income of less than $100,000 (OR 0.74, CI 0.31-1.75). Patients who developed complications were more likely to have comorbid renal failure (OR 1.82, CI 1.03-3.03) or congestive heart failure (OR 2.65, CI 1.31-5.36) Conclusion Patient race and income are not strongly correlated with rates of wound dehiscence, seroma, hematoma, or infection within 30 days of chest wall plastic reconstruction. However, male patients have a higher rate of complications than female patients, and patients who develop complications are more likely to have comorbid renal failure or congestive heart failure. These findings contribute valuable insights into wound healing dynamics. Investigation into these factors could pave the way for novel therapeutic approaches and improved wound management strategies.

.jpeg)
