Health Economics
(HE-007) Comparing inpatient cost and number of readmissions for infections, debridement, and/or dehiscence by severity of illness for 7 admission procedures
The aim of this study was to improve our understanding of the economic implications related to treating moderate and major severity of illness (SOI) patients for chronic wound infections causing readmissions.
Methods:
Using a retrospective cohort design, this study utilized data from the Centers for Medicare and Medicaid Services Longitudinal Data Set Standard Analytic Files (CMS LDS SAF) from 2017-2021. We examined the number and cost of inpatient readmissions to Level 1 Trauma Centers in the United States among patients originally admitted for 7 high-risk procedures (diabetic foot ulcers, pressure ulcers, skin grafts and flaps, total hip arthroscopy, femoral popliteal bypass procedures, coronary artery bypass graft [CABG] and valve procedures, and spinal fusions) who also had potentially preventable readmissions for infections, dehiscence, or debridement. Data were disaggregated by SOI (according to 4 measurable classification levels: mild, moderate, major, and extreme) for the initial admission.
Results:
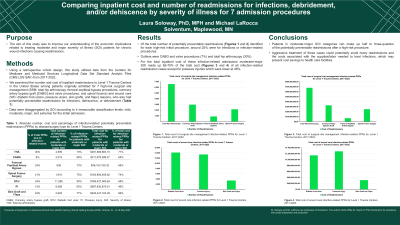
Of the total number of potentially preventable readmissions identified for each high-risk initial procedure, around 25% were for infections or infection-related procedures. Outliers were CABG and valve procedures (7%) and total hip arthroscopy (30%). For the total inpatient cost of these infection-related admissions, moderate+major SOI made up 65-75% of the total cost of all infection-related readmission cases (except for pressure injuries which were lower at 46%). When looking at the number of infection-related admissions, the range for moderate+major SOI was 64-80%.
Discussion:
Patients in moderate+major SOI categories can make up half to three-quarters of the potentially preventable readmissions after a high-risk procedure. Aggressive treatment of these cases could potentially avoid many readmissions and the costs associated with the supplies/labor needed to treat infections, which may present cost savings to health care facilities.

.jpeg)
